Hepatitis B: As Few as Two Shots for a Lifetime of Protection
Jan 16, 2019, 11:01 AM
by Leslie Kolb, RN, BSN, MBA, AADE Chief Science and Practice Officer and
William Schaffner, MD, NFID Medical Director, Vanderbilt University School of Medicine
Vaccine recommendations by the Centers for Disease Control and Prevention (CDC) are not made lightly. When CDC says that everyone age 60 years and younger with diabetes needs to be immunized against hepatitis B, it is because they are at increased risk of infection from the hepatitis B virus (HBV) and once they have it, are at further risk of serious outcomes.
Let’s start with the risk of infection. People with diabetes have twice the odds of becoming infected with HBV compared to those without the disease. HBV is blood borne and among the causes of increased risk for people with diabetes is improper equipment use during blood glucose monitoring.
In adults without diabetes, there is a one in 20 chance that their HBV infection will become chronic. But the risk of chronic infection is higher for a person with diabetes. This matters because chronic HBV infection is serious and deadly.
HBV attacks the liver silently at first and most people don’t know they are infected until a few decades later when symptoms appear. By the time they are aware, the virus has done extensive damage and eventually two out of every five people will end up with liver cirrhosis, liver failure or liver cancer. Some may require extensive drug treatment or liver transplant and one in four will die prematurely.
Although chronic infection is the bigger concern—far fewer adults will suffer serious health consequences in the acute, or early, stages of infection. But even here, people with diabetes do worse than their counterparts without diabetes. Data from the CDC Emerging Infections Program collected in 2009-2010 reported a fatality rate of 5 percent among adults with diabetes during the early days of HBV infection compared with 2 percent among adults without diabetes.
Vaccinate to avoid HBV infection—nothing else works nearly as well!
Evidence of past hepatitis B infection is high among people with diabetes—60 percent higher than among adults without diabetes.
Two-thirds of US adults with chronic infection have no idea they have it, and with up to 2.2 million infected, that is a lot of people transmitting a virus they may not know they have.
After years of HBV infections declining in the US thanks to widespread vaccination among children, there is evidence that infection rates are now on the rise again. It appears this is due to a combination of far too many adults not being vaccinated along with increasing rates of injection drug use connected with the opioid crisis.
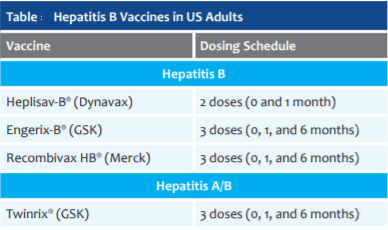 Here’s what does work: vaccination! There are three very effective and safe hepatitis B vaccines approved for use in adults in the US (see Table). There is also a combination vaccine that protects against both hepatitis A and B. The newest of the hepatitis B vaccines, Heplisav-B®, is administered as a two-dose series, one month apart. The other vaccines, Engerix-B®, Recombivax HB® and Twinrix® are administered as a three-dose series with the first two doses also one-month apart and then a third dose at six months.
Here’s what does work: vaccination! There are three very effective and safe hepatitis B vaccines approved for use in adults in the US (see Table). There is also a combination vaccine that protects against both hepatitis A and B. The newest of the hepatitis B vaccines, Heplisav-B®, is administered as a two-dose series, one month apart. The other vaccines, Engerix-B®, Recombivax HB® and Twinrix® are administered as a three-dose series with the first two doses also one-month apart and then a third dose at six months.
The three-dose vaccines protect more than 90 percent of adults younger than age 40 and 74 percent of adults age 60 and older. The newer two-dose vaccine protects more than 90 percent of adults between 18 and 70 years old, with protection more than 90 percent even in the 60 to 70-year-old age range. While three-dose vaccines are less effective in adults with diabetes, Heplisav-B® provides similar protection for those with and without diabetes.
Final thoughts
The hepatitis B virus is like a submarine—silent but deadly. The virus is 50 to 100 times more infectious than HIV and it can live outside the body for at least seven days and still be capable of causing an infection. It can also be transmitted in the absence of visible blood. It can infect anybody and lead to serious illness and even premature death, but people with diabetes are at particularly increased risk of getting infected and having worse outcomes.
The latest CDC statistics indicate that at best, only one in four people with diabetes is vaccinated as recommended. That means as a healthcare provider, your strong recommendations and reminders about this vaccine are vital—three out of every four people you counsel will need to hear you. Their lives may literally depend on it.
Access guidance on vaccinations for people with diabetes and other resources at DiabetesEducator.org/vaccination and www.nfid.org.